Slideshow Items
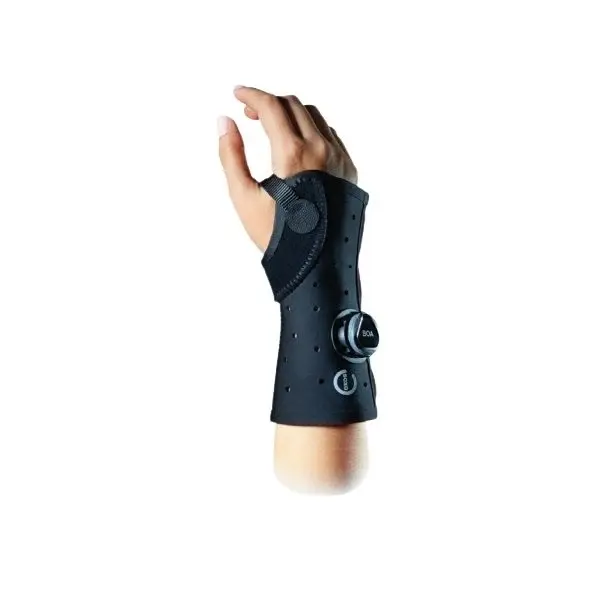
The Exos Brace Molding Service is a professional clinical heat molding and custom anatomical fitting service for EXOS thermoformable orthopedic braces to ensure personalized anatomical fit, optimal immobilization, and pressure-point relief.
EXOS braces are manufactured from a proprietary thermoformable polymer composite that softens and becomes pliable when heated to a specific temperature range — typically between 60 and 75 degrees Celsius — and returns to a rigid, shape-retaining structure as it cools to body and room temperature. This thermoplastic behavior is the material property that distinguishes EXOS from conventional rigid orthoplastic braces and from soft neoprene or fabric braces at the other end of the immobilization spectrum. A conventional rigid brace is manufactured in a fixed geometry that approximates the average anatomy of its size category — it cannot be altered to accommodate the patient's specific bony prominences, joint angles, or limb contours, and the clinical consequence is a brace that fits well for the statistical average patient and poorly for everyone whose anatomy deviates from that average. The EXOS thermoformable system is engineered to be clinician-molded to each individual patient's anatomy — but that molding capability is only realized when the heat molding process is performed correctly by a trained clinician with appropriate heating equipment and anatomical positioning knowledge.
The heat molding process involves controlled heating of the EXOS brace panel in a specialized dry heat oven or heat gun until the polymer reaches its thermoplastic transition temperature, confirmed by the material becoming visibly translucent and pliable under gentle manual pressure. The clinician then applies the heated brace to the patient's limb in the prescribed therapeutic position — maintaining the joint angle and alignment specified by the treating physician or therapist — and uses controlled manual pressure to conform the softening polymer to the patient's bony landmarks, contour transitions, and soft tissue topography. As the material cools — typically over 3 to 5 minutes of maintained positioning — it solidifies into a three-dimensional shell that precisely reproduces the patient's anatomy in the therapeutic position. The result is a brace whose inner surface contacts the patient's limb uniformly across the full contact area rather than at isolated prominence contact points — distributing the immobilization force over the widest possible tissue area and eliminating the concentrated interface pressure at bony prominences that causes pain, skin breakdown, and compliance failure in improperly fitted braces.
The clinical significance of pressure point elimination in orthopedic brace fitting extends beyond patient comfort into therapeutic effectiveness and compliance. A brace that creates significant pressure discomfort at bony prominences — the ulnar styloid in wrist braces, the lateral malleolus in ankle braces, the first metatarsal head in foot braces — will be removed by the patient during the hours when it causes the most discomfort: typically at night and during sedentary activities when the immobilization is least practically inconvenient to remove but most therapeutically important for fracture healing or soft tissue recovery. Patient-reported brace removal rates in improperly fitted rigid orthoses are substantially higher than in custom-molded equivalents — and the cumulative hours of brace non-use during a recovery period directly affect the healing outcomes the brace is prescribed to protect. A correctly heat-molded EXOS brace that distributes interface pressure uniformly across the full contact surface is worn continuously because it is not uncomfortable enough to justify removal — and consistent wear is the fundamental prerequisite for the brace to achieve its therapeutic function.
The remoldability of the EXOS thermoformable system is a clinical advantage that conventional rigid braces cannot offer and that is particularly valuable in the management of fractures and post-operative limb conditions where tissue swelling follows a predictable resolution trajectory over the first two to four weeks of recovery. At the time of initial fitting — typically within 48 to 72 hours post-injury or post-surgery — limb circumference is at its maximum due to acute inflammatory swelling, and the brace is molded to this swollen limb geometry. As swelling resolves over the following weeks, the limb circumference decreases and the brace that was correctly fitted to the swollen limb becomes progressively looser — the contact surface area decreases, concentrated pressure points re-emerge at the remaining contact sites, and the brace provides less immobilization as the limb-to-brace contact force distribution deteriorates. With an EXOS thermoformable brace, the clinician can reheat the brace at a follow-up appointment and remold it to the patient's reduced limb circumference, restoring the uniform contact surface and immobilization quality that was achieved at initial fitting — a capability that makes a single brace appropriately sized throughout the full swelling-resolution recovery period.
✓ Wrist fractures — distal radius, scaphoid, and carpal fractures requiring custom-molded immobilization in the prescribed wrist position throughout the healing period ✓ Wrist sprains and ligament injuries — TFCC, scapholunate, and lunotriquetral ligament injuries requiring immobilization in functional wrist position ✓ Thumb injuries — ulnar collateral ligament sprains, Bennett fractures, and first CMC joint instability requiring custom thumb spica or post molding ✓ Foot and ankle stabilization — post-fracture or post-ligament injury ankle and midfoot immobilization where standard Walker boot fit is insufficient ✓ Post-operative orthopedic support — wrist, hand, ankle, and foot surgical sites requiring custom immobilization in the surgically determined position during early healing ✓ Sports injury management — athletic injuries where return-to-training timelines require a brace that is both therapeutically effective and comfortable for activity ✓ Pediatric fracture management — children's limb proportions and smaller anatomy benefit particularly from custom-molded rather than size-category-based brace fitting ✓ Chronic joint instability — recurrent wrist or ankle instability where a comfortable, precisely fitting brace supports proprioceptive protection during activity ✓ Occupational injury rehabilitation — workplace injury cases where brace compliance is a documented outcome measure in return-to-work timelines ✓ Patients with atypical limb anatomy — post-surgical scar tissue, previous fracture deformity, or anatomical variation that standard brace sizes cannot accommodate
Pre-Molding Assessment Before initiating the heat molding process, the clinician reviews the treating physician's or therapist's prescription for the specific brace model, therapeutic joint position, and any immobilization precautions relevant to the patient's diagnosis. The clinician measures the patient's limb circumference and joint dimensions to confirm the EXOS brace size is correct — a brace that is too small cannot be molded to cover the required anatomical area regardless of heat molding technique, and a brace that is significantly oversized will have excess polymer volume that creates bulk and weight without additional immobilization benefit. The clinician identifies the key bony landmarks that will require relief in the molding — the ulnar styloid for wrist braces, the lateral malleolus for ankle braces, the first metatarsal head for foot braces — and plans the molding sequence to ensure these areas are addressed during the critical shaping window.
Testimonial items
Very welcoming and informative. We went in to rent a Walker for my mom to see if she would use it. They had no rentals left so he gave us a brand new one on rental. Highly recommend this company for all your ADL needs.
Tara Maye
The rating of this product is 5 out of 5
Fantastic service and experience, from delivery to pickup we could not have asked for anything more! We rented a hospital bed, and I do not believe you would get better service anywhere. Highly recommended!
Shawn Dillon
The rating of this product is 5 out of 5
Super friendly and very helpful! Delivered the wheelchair for me, special ordered other parts and took the time to show me how to install. I recommend!
Fiona Haines
The rating of this product is 5 out of 5
Can not thank the team at Med Supplies enough for their amazing service. We were in a tough spot till we got their help. Amazing service. Kind and respectful delivery. First class all the way. Thank you again.
Jon Beatty
The rating of this product is 5 out of 5
Ordered the chair on Sunday and it arrived Monday morning. Spoke to customer service to follow up on delivery times. It was already on my front door. Excellent and helpful staff. The product is sturdy and of good quality. Thank you for your help.
H D
The rating of this product is 5 out of 5
Excellent experience - website faithfully represented what was in stock (which hasn't always been my experience with other vendors sadly), and local shipping was really fast - ordered on the weekend, received it on Monday in my case. Thank you for being
Jason Hudson
The rating of this product is 5 out of 5
0/0
You cart is currently empty
 780 409-1509
780 409-1509 Get directions
Get directions